Health Insurance
45% of Insured Americans Considering Health Insurance Changes During Open Enrollment

This open enrollment season, many are contemplating making changes to their health insurance coverage. According to the latest ValuePenguin survey of 1,795 Americans with health insurance, 45% are considering switching their plan or coverage provider or changing the amount of coverage. Most commonly, those looking to change their health insurance are doing so in response to the COVID-19 pandemic (35%) or their transforming health needs (33%).
Additionally, 27% of consumers are considering changing their health insurance coverage for cost-related reasons. For 18% of this group, the driving force is that out-of-pocket costs were too high last year. Another 9% of people feel they pay for more insurance than what they use, so they're seeking to cut back on expenses.
As concerns about cost sit at the forefront for many insured Americans, nearly half (46%) expect health insurance to be even more expensive in 2022. While cost-related factors are already leading 27% of consumers to reconsider their health care insurance coverage, 40% of people felt their out-of-pocket costs were too high — with almost 20% unable to afford their deductibles.
Key findings
- 45% of insured Americans are considering changes to their health insurance during open enrollment, namely switching the plan provider or type. Those with marketplace plans are most often looking to make a change. The coronavirus pandemic is the main reason consumers are changing their health insurance, followed by changing health needs and dissatisfaction with their provider.
- As nearly half of Americans (46%) expect higher health insurance premiums in 2022, some struggle to afford health care costs. 4 in 10 insured Americans say their out-of-pocket health care costs were too high in the last year, and nearly 1 in 5 say they can’t afford their deductible.
- 45% of insured Americans believe those who aren’t vaccinated for COVID-19 should pay higher health insurance premiums than those who are vaccinated. This sentiment is highest among baby boomers (ages 56 to 75) at 53%.
- Premium costs are the most important factor Americans consider when selecting a health insurance plan, at 24%. Services covered (20%) and deductibles (14%) are other decision drivers.
- 24% of Americans have made a mistake during open enrollment before. The most common errors shoppers committed were not fully exploring their options (28%) and missing the deadline for open enrollment (26%). About one-third of Gen Zers (ages 18 to 24) and millennials (ages 25 to 40) made mistakes during open enrollment.
Nearly half of insured consumers are thinking about making a change to their health insurance coverage this year, with young people being the most open to a switch
Forty-five percent of insured shoppers are considering reevaluating their health insurance coverage during this year's open enrollment season. Twenty-two percent of these people are still deciding which part of their insurance coverage they want to change, but 23% have zeroed in on at least one element of their current policy with which they're dissatisfied. Most of these people want to find a new health insurance plan type or switch to another health insurance provider altogether — 8% for both.
Gen Zers are the most likely to want to change their health insurance. Forty-three percent of Gen Zers will change their coverage, while another 20% are still considering it. Thirty-eight percent of people in this age group are set on not changing their health insurance coverage this year — the lowest compared to any other group.
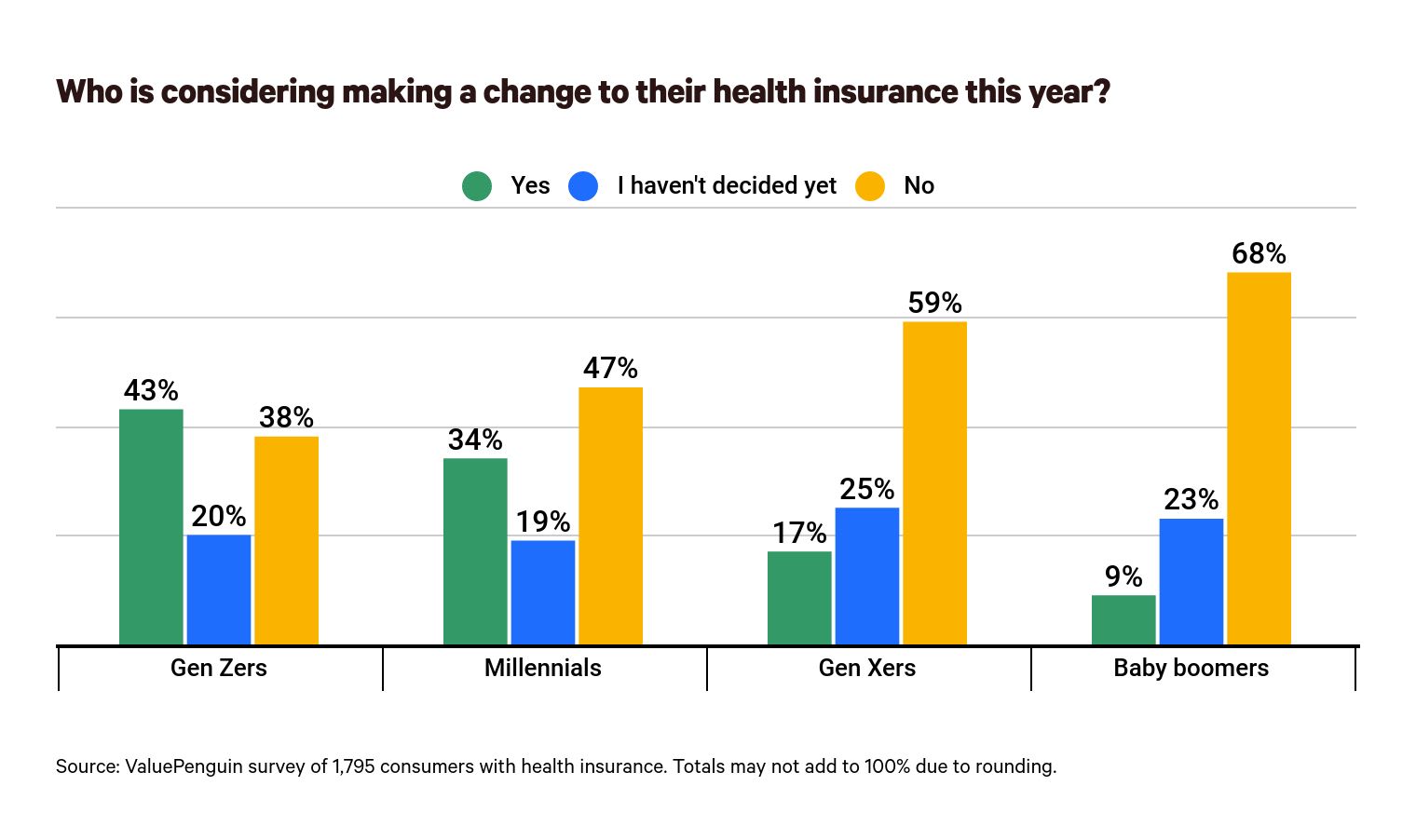
Baby boomers are the least likely to change their health insurance. Sixty-eight percent of people from this group have already decided they won’t change their coverage this year. Sixty-two percent of those with Medicare (which insures those 65 or older, among other high-risk groups) or other public forms of health insurance aren’t considering a change this year. By comparison, those with marketplace plans are most likely to consider a change as just 27% of these people won't adjust their health insurance coverage this year.
What's driving people to change their health insurance?
The pandemic influenced the decisions of many to consider switching up their health insurance.
COVID-19 is a factor for 35% of people thinking about changing their health insurance this year — the most of any other cause. Demographically, 44% of millennials considering changing their health insurance cite the pandemic as a factor, the highest percentage of any group. COVID-19 most frequently affected the decisions of those with kids younger than 18 — 44% of these parents considering changing their coverage identified the pandemic as a factor.
Reason | Total | Gen Zers | Millennials | Gen Xers | Baby boomers |
|---|---|---|---|---|---|
| The coronavirus pandemic | 35% | 38% | 44% | 25% | 5% |
| Health needs have changed | 33% | 37% | 31% | 33% | 34% |
| Not satisfied with current plan or provider | 25% | 24% | 24% | 29% | 25% |
| Out-of-pocket costs too much last year | 18% | 20% | 19% | 13% | 21% |
| Overinsured and paying for unused coverage | 9% | 19% | 5% | 13% | 5% |
| Life event (marriage, baby, etc.) | 9% | 4% | 11% | 10% | 7% |
| Other | 6% | 1% | 3% | 11% | 16% |
Source: ValuePenguin survey of 1,795 consumers with health insurance.
Behind the pandemic, the leading factor bringing people to consider changing their health insurance is experiencing a change to their health needs. Thirty-three percent of people identify this as an influence. Other common answers include dissatisfaction with their current plan (25%) and high out-of-pocket expenses (18%). With this segment, another 9% feel they’re paying too much for services they don't use. Cost, then, plays a part for 27% overall.
46% of insured consumers expect health insurance to be more expensive in 2022, even while 40% already believe their out-of-pocket costs are too high
While 27% of insured people considering changing their health insurance coverage cite cost-related factors as decision drivers, more than 4 in 10 consumers expect health insurance prices to rise in 2022 — and this is likely. Personal out-of-pocket costs have gone up by 103% since 2001, totaling $7.9 trillion in expenses. To underscore the severity of rising costs, 40% of consumers already say their out-of-pocket costs are too expensive.
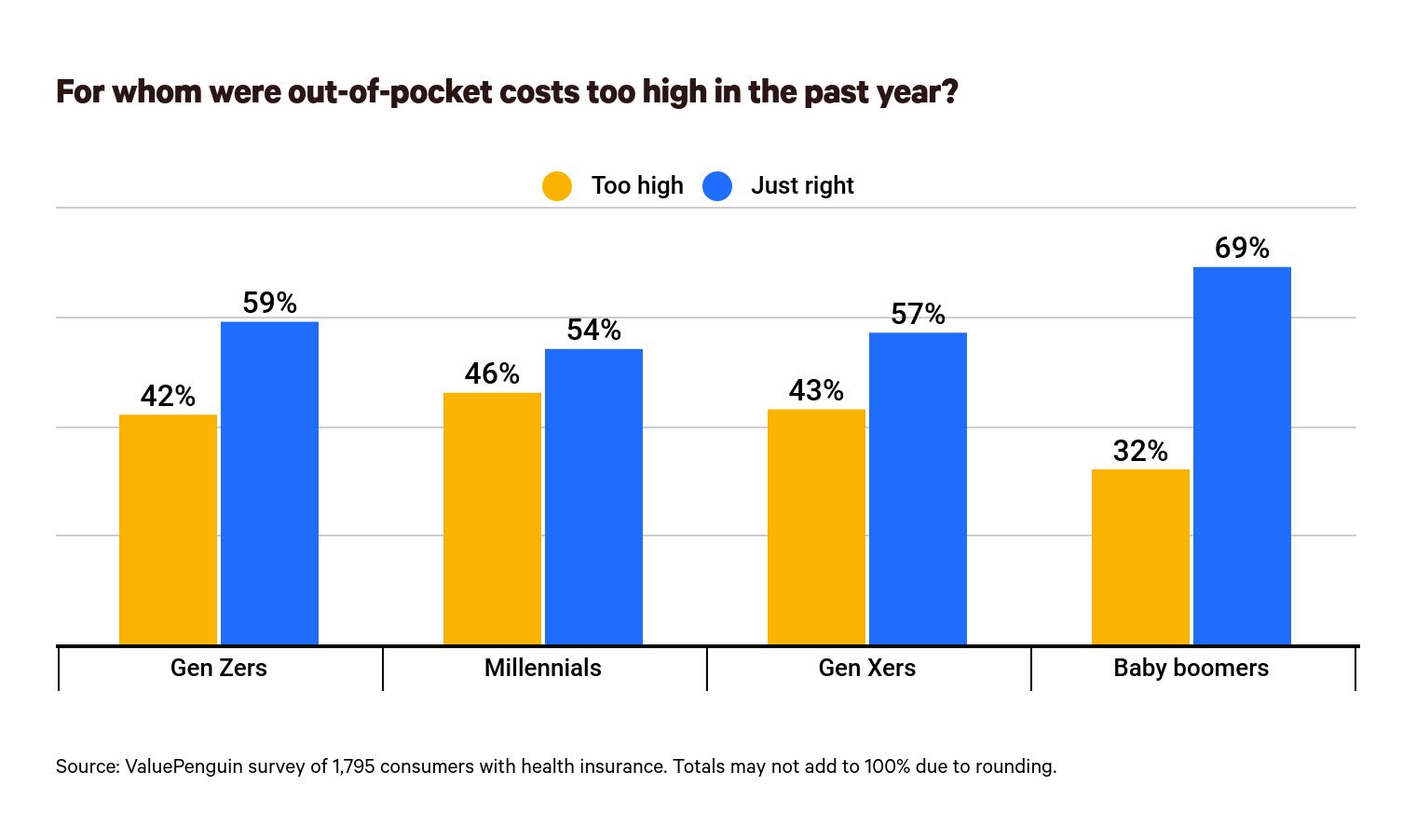
Among these 40% of people who think they pay too much for health insurance, millennials are most likely to believe that their out-of-pocket costs — including deductibles, copays, coinsurance payments and uncovered services — are too expensive (46%). Conversely, 32% of baby boomers believe their out-of-pocket costs are too high, the lowest of any group.
Baby boomers are most likely to believe that unvaccinated people should be charged more for health insurance. Fifty-three percent of insured Americans in this demographic support higher rates for the unvaccinated. For comparison, 45% of all insured consumers support charging unvaccinated people more. At 40% support, Gen Xers are the least likely of any age group to favor this type of markup.
ValuePenguin also asked consumers about their deductibles, an out-of-pocket cost that can be expensive. Deductibles for health insurance — the amount paid per year for medical services before cost-sharing starts — can total thousands of dollars a year. Eighteen percent of insured people can’t afford their deductibles, including one-fourth of Gen Zers. Another 20% of consumers don't know their deductible amounts.
For 14% of insured people, their deductible is the most important point to consider when comparing health insurance plans. More broadly, out-of-pocket costs take priority for 12% of consumers. For most (24%), however, monthly premiums are the most important thing to consider when selecting health insurance coverage.
Factor | Total | Gen Zers | Millennials | Gen Xers | Baby boomers |
|---|---|---|---|---|---|
| Monthly premium cost | 24% | 24% | 26% | 22% | 22% |
| Services covered | 20% | 22% | 18% | 20% | 22% |
| Deductible | 14% | 16% | 17% | 14% | 10% |
| Out-of-pocket costs | 12% | 12% | 10% | 13% | 14% |
| Provider/network | 11% | 8% | 10% | 12% | 14% |
| Copay | 11% | 15% | 14% | 11% | 7% |
| Prescription costs | 6% | 4% | 4% | 6% | 6% |
| Other | 2% | 2% | 1% | 1% | 5% |
Source: ValuePenguin survey of 1,795 consumers with health insurance.
Millennials are most likely to view the cost of a policy as the most important factor when selecting a health insurance plan. More than one-quarter (26%) of this age group prioritize monthly premiums, and 17% believe deductibles are the most important quality. Baby boomers are the most likely to focus on out-of-pocket costs (13%), and 15% of Gen Zers care most about their copays — the largest percentage of any group concerned about this.
Almost 1 in 4 shoppers has made a mistake during open enrollment, with young people being the group most prone to errors
During open enrollment, consumers can change their health insurance coverage preferences. While most people have never made a mistake around open enrollment, nearly one-quarter of consumers have — including about one-third of Gen Zers (32%) and millennials (33%).
Most frequently, shoppers didn't take enough time to compare their options. Twenty-eight percent of shoppers didn’t fully explore their options, ahead of people who didn't purchase enough coverage (17%) and those who bought too much (14%). Twenty-six percent of consumers who made mistakes, however, missed the deadline for open enrollment entirely.
ValuePenguin encourages shoppers to compare premiums, copays, deductibles and other costs of a few plans before purchasing one. Consumers should also be aware of their out-of-pocket maximums, the amount of money a policyholder has to spend a year before their insurance covers all costs.
Avoid missing the window for open enrollment this year. The start of open enrollment for 2022 marketplace health insurance coverage started Nov. 1 and goes until Dec. 15. Some people — those who’ve experienced a life event or who’ve changed residences or lost their insurance — may qualify for special enrollment status and sign up after Dec. 15, with a Jan. 15 deadline a month later.
Methodology
ValuePenguin commissioned Qualtrics to conduct an online survey of 1,795 U.S. consumers who have health insurance, from Oct. 15-20, 2021. The survey was administered using a non probability-based sample, and quotas were used to ensure the sample base represented the overall population. All responses were reviewed by researchers for quality control.
We defined generations as the following ages in 2021:
- Generation Z: 18 to 24
- Millennial: 25 to 40
- Generation X: 41 to 55
- Baby boomer: 56 to 75
While the survey also included consumers from the silent generation (those 76 and older), the sample size was too small to include findings related to that group in the generational breakdowns.

