What Is a Health Insurance Deductible and How Does It Work?
Your deductible is the amount you have to pay for health care bills before your plan starts to pay.
Find Cheap Health Insurance Quotes in Your Area
Health insurance deductibles are annual, which means you have to pay the deductible each year. When you reach your deductible, your health insurance plan will start paying toward your medical bills until the end of the year.
What is a deductible in health insurance?
A health insurance deductible is the amount of money you have to pay toward your medical bills yourself before your plan starts to pay.
For example, if you have a plan with a $1,500 deductible, you have to pay $1,500 toward your medical bills each year, and then your plan will start paying part of your bills.
Usually, your health insurance will pay for things before you reach your deductible. For example, nearly all health insurance plans completely pay for things like annual checkups, vaccines and cancer screenings. Even if you haven't met your deductible, you shouldn't have to pay anything for these kinds of care.
With other types of care, you might pay a flat rate, called a copay, even if you haven't yet reached your deductible. For example, you might only pay $20 to go to a doctor's office or urgent care, or $50 to go to the emergency room.
Unlike home and car insurance deductibles, which you have to pay every time you file a claim, health insurance deductibles are annual. That means you only have to reach your deductible once during each calendar year.
Once you reach your deductible, you and your health insurance plan start splitting your bills. You'll usually pay a percentage of your medical bills, called coinsurance.
So if your plan has a $1,000 deductible and you have a medical bill that costs $4,000, you'll pay the first $1,000. After that, you'll split the remaining $3,000 with your health insurance company. You might pay 20% of the $3,000 balance, which is $600, while your health insurance company pays $2,400.
Types of health insurance deductibles
There are a few different types of health insurance deductibles, and sometimes your plan can even have more than one deductible. For example, you might have separate deductibles for medical bills and prescription medications. It's also common to have separate deductibles for in-network doctors and out-of-network doctors.
Some health insurance plans have a separate deductible for prescription medications. That means you have to pay a set amount toward your medications, separate from the amount you pay toward your medical bills, before your plan starts paying.
People who take expensive medications may actually benefit from having a separate prescription deductible. That's because drug deductibles are usually lower than medical deductibles. For a Silver health insurance plan, the average medical deductible is $4,367. But for plans that have separate deductibles for medical care and prescriptions, the average drug deductible is just $1,700.
Certain types of health plans, called PPO and POS plans, cover you to get medical care from both in-network and out-of-network doctors. But you'll pay more if you go outside the network. That's because there are usually higher deductibles for out-of-network doctors. PPO and POS plans give you the flexibility to go to any doctor, but you'll still save money if you stick to in-network offices.
If you have an HMO or EPO plan, you won't have any coverage for out-of-network doctors or medical offices. You won't have an out-of-network deductible because out-of-network care isn't covered at all, except in emergencies. That means you have to pay the full cost for any medical care you get outside the plan's network.
If your health insurance plan just covers you, your deductible will just be for your medical care. This is called an "individual deductible."
But if you have more than one person on your health insurance plan, like a spouse or children, your plan works a bit differently. You'll need to check whether you have what's called "embedded" or "nonembedded."
With an embedded deductible, each person in the family has an individual deductible and the entire family has an overall family deductible. Your health insurance company tracks how much you pay toward medical bills for each person as well as how much you pay for everyone's medical care in total.
If your plan has an embedded deductible, your company starts to pay toward your medical bills when one of two things happens:
- As soon as one person reaches their individual deductible, the company starts paying toward the medical bills for that person only.
- If the entire family reaches the family deductible, the plan pays toward everyone's medical bills for the rest of the year. This happens even if some family members haven't reached their individual deductibles.
In a nonembedded plan, you'll only have a family deductible. That means everyone's medical bills are pooled together. Once the family deductible is met, the plan starts paying toward everyone's medical bills.
How to choose a deductible
To pick the best health insurance deductible, think about your monthly budget, health care needs and overall financial health.
In general, the higher your deductible, the cheaper a health insurance plan will be each month. That's why lower-tier plans like Bronze have cheaper rates than higher-tier plans like Gold. If getting a cheap plan is your top priority, choosing a higher deductible will help keep your rates low.
Find Cheap Health Insurance Quotes in Your Area
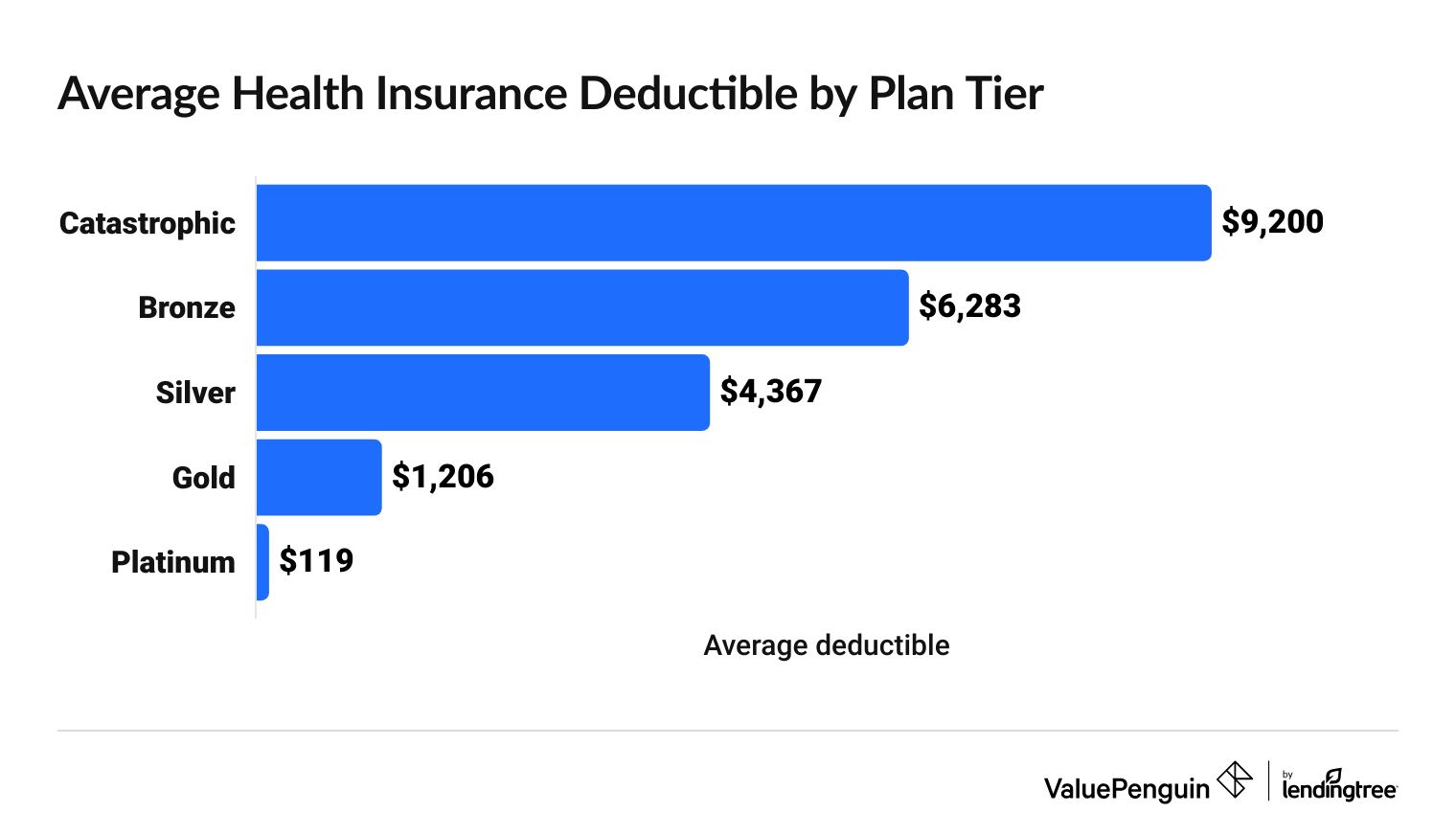
Health insurance deductibles and rates by plan tier
Plan tier | Average deductible | Monthly rate |
|---|---|---|
| Catastrophic | $9,200 | $361 |
| Bronze | $6,283 | $488 |
| Silver | $4,367 | $621 |
| Gold | $1,206 | $676 |
| Platinum | $119 | $913 |
Average monthly rates are for a 40-year-old.
But you should always make sure you can afford the deductible, in case something serious happens. If you break your leg and need surgery, you might end up having to pay your deductible all at once. If you can't afford that, you might have to take out a loan.
If you go to the doctor often, know you'll need surgery, or have a chronic or complex medical condition, picking a plan with a lower deductible is usually a good idea.
The lower deductible means you'll probably pay less overall because your plan will pay for a bigger share of your medical bills. But lower-deductible plans cost more, so you need to make sure you can afford the higher monthly rate.
Frequently asked questions
How do deductibles work for health insurance?
Your deductible is the amount of your medical bills you have to pay yourself before your health insurance starts paying. So when you get bills for medical treatment, you have to pay them until you reach your deductible. At that point, your health insurance will start splitting the bills with you.
Do copays count toward my deductible?
Copays, which are flat fees that you pay for some medical care, don't usually count toward your deductible. However, copays do count toward your out-of-pocket maximum. Once you hit your out-of-pocket maximum, your health insurance pays for all of your covered medical care.
Is it better to have a high or low deductible for health insurance?
If you need frequent or expensive medical care, paying more for a low-deductible plan can help you save money overall, even though the plans are more expensive. If you're mostly healthy, a high deductible can be a good way to save money on your monthly health insurance rate. But you should make sure you can afford the high deductible if something serious happens.
Methodology and sources
Average health insurance rates and deductibles come from the Centers for Medicare & Medicaid Services (CMS) public use files (PUFs) and state health insurance marketplace websites. All rates are for a 40-year-old.
About the Author

Senior Writer
Licensed Insurance Agent
Cate Deventer is a Senior Writer who specializes in health insurance, Medicare, auto and home insurance. She's been a licensed insurance agent since 2011.
She started her insurance career working as a customer service agent for State Farm. She later moved to an independent agency, where she worked with several insurance companies and hundreds of clients. She quoted policies, filed claims and answered insurance questions. In 2021, she pivoted her career and began writing about insurance for Bankrate. She moved to ValuePenguin in 2023 and began writing about health insurance and Medicare.
Cate has a passion for helping readers choose insurance to fit their needs. She enjoys knowing that her research and knowledge help people choose insurance products that make a positive difference in their lives.
How insurance helped Cate
Cate used her health insurance knowledge to navigate a surgery in 2023. Understanding how her policy worked let her focus on recovery instead of worrying about bills.
Expertise
- Health insurance
- Medicare & Medicaid
- Auto insurance
- Home insurance
- Life insurance
Credentials
- Licensed Life, Accident & Health Insurance Agent
- Licensed Property & Casualty Insurance Agent
Referenced by
- CBS
- NBC
- Wall Street Journal
Education
- BA, Theatre, Purdue University
- BA, English, Indiana University
Editorial note: The content of this article is based on the author's opinions and recommendations alone. It has not been previewed, commissioned or otherwise endorsed by any of our network partners.
