When Does Medicaid Cover Dental Care?
Medicaid always covers some dental care for children and young adults under 21, but coverage for adults over 21 depends on where you live.
Find Cheap Health and Dental Insurance Quotes in Your Area
That's because Medicaid gets its funding from both the federal government and the states. The federal government sets some rules that all states have to follow, like making sure people under 21 can get dental treatment. But states have some freedom to customize their Medicaid programs, which is why dental care for adults depends on where you live.
Also on this page:
Medicaid dental coverage for children and young adults
Medicaid is required to cover some kinds of dental care for kids and young adults under the age of 21.
Under Medicaid, dental services for children and young adults can't be limited to emergency care. The services must be comprehensive and be covered often enough to follow normal dental care standards.
By law, state Medicaid programs have to cover at least three types of dental care for people under 21:
- Dental health maintenance
- Pain and infection treatment
- Tooth restoration
This means Medicaid covers preventive dental care such as check-ups, cleanings and x-rays. It also covers restorative services such as fillings, crowns, root canals, oral surgery and emergency procedures.
Additionally, if a dental condition is discovered during a dental exam, the state Medicaid program has to provide the necessary care to treat that condition. That's true even if the state doesn't usually cover that specific treatment.
Dental care is considered part of Medicaid's Early and Periodic Screening, Diagnostic and Treatment (EPSDT) benefit, which is aimed at prevention and early diagnosis of medical conditions, so they can be treated more effectively.
Medicaid dental coverage for adults
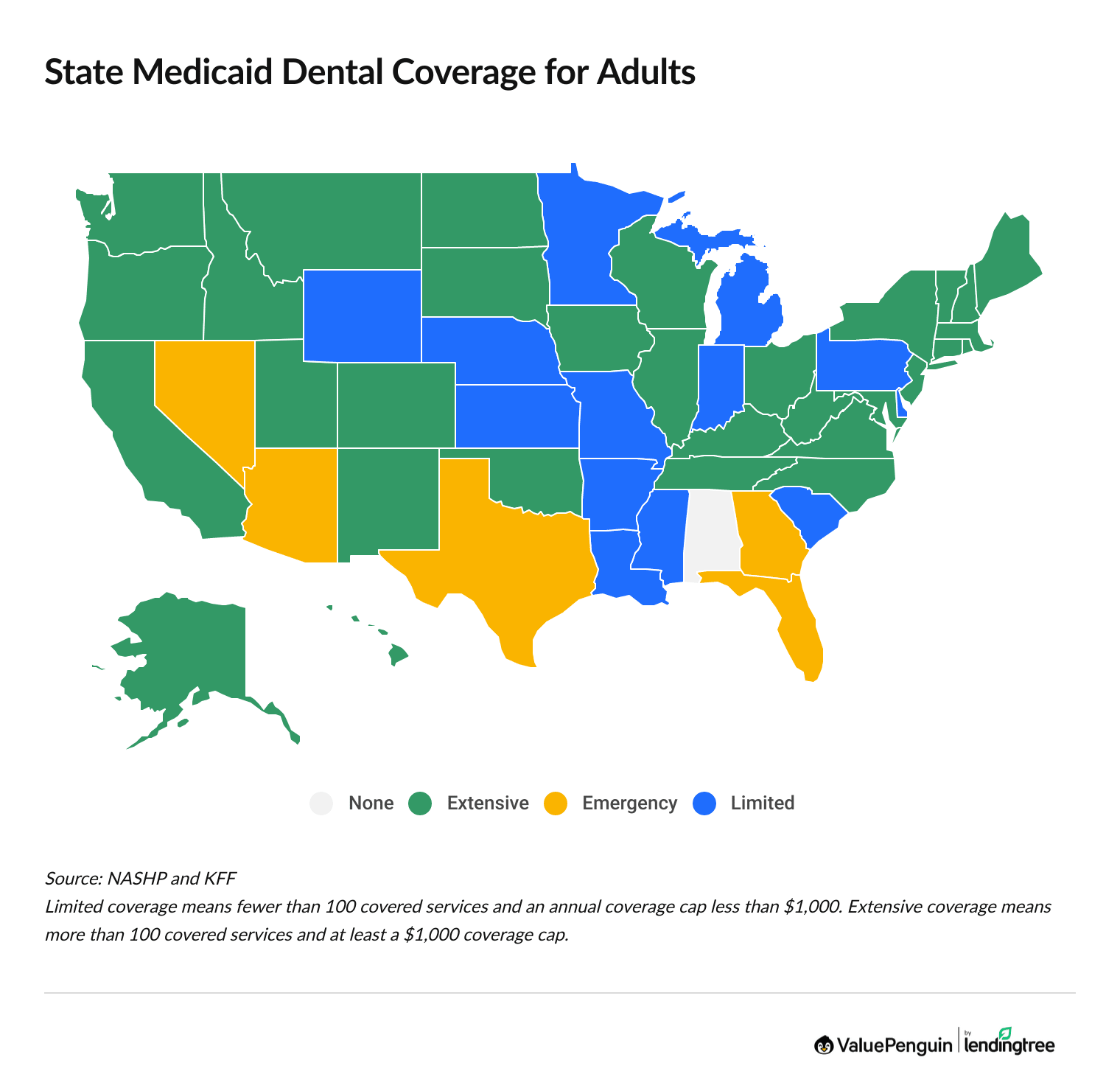
Every state except Alabama offers some kind of dental coverage for adults on Medicaid.
However, the level of coverage changes depending on where you live. In Arizona, Florida, Georgia, Nevada and Texas, only emergency dental coverage is available from Medicaid. In 13 other states, coverage is limited to only a few services. But in 31 states and Washington, D.C., dental coverage for adults is fairly broad. The exact coverage varies by state but often includes cleanings, fillings, root canals and sometimes even dentures.
Find Cheap Health and Dental Insurance Quotes in Your Area
Some state Medicaid programs have limits on annual dental care. For example, in Alaska, adults on Medicaid are covered for things like cleanings, crowns and even dentures, but only up to $1,150 per year. If you live in a state with a coverage cap, it means you have to pay the full cost for dental care if you go over the limit.
State Medicaid laws are subject to change at any time. The info here is accurate as of July 2025, but states can add or remove dental coverage for adults as they see fit. Contact your state's Medicaid office for more info on your state's dental coverage for adults.
Adult Medicaid dental coverage by state
State | Medicaid dental coverage for adults |
|---|---|
| Alabama | None |
| Alaska | Extensive |
| Arizona | Emergency |
| Arkansas | Limited |
| California | Extensive |
Source: NASHP and KFF. Limited coverage is fewer than 100 dental care services and an annual coverage cap of less than $1,000. Extensive coverage is more than 100 covered dental services and an annual cap greater than $1,000. The definitions are from The National Academy for State Health Policy (NASHP) and adapted from the Center for Health Care Strategies and American Dental Association Health Policy Institute.
Medicaid dental coverage during pregnancy
Many Medicaid programs make it easier for pregnant women with low incomes to get dental care.
This means that in some states where dental coverage is limited for most adults, pregnant women can still get care. In Michigan, for example, most adults on Medicaid only get limited dental coverage. But pregnant women have access to more extensive coverage. It's also usually easier to get Medicaid when you're pregnant, because the income limits are higher. That means you can make more and still qualify.
Will Medicaid pay for dental implants?
In most cases, Medicaid does not cover dental implants.
Medicaid usually considers dental implants a cosmetic procedure and not medically necessary. However, if you and your dentist can prove that the implants are necessary, Medicaid might pay for them. And in states where dental coverage for adults is extensive, you might have coverage for dentures.
How to find a dentist that accepts Medicaid
Only about 1 in 3 dentists nationwide accept Medicaid.
If you have Medicaid, there are a few places you can go to find a dentist that takes your coverage.
- Children: The government website InsureKidsNow.gov is one of the best places to find a dentist who accepts Medicaid or the Children's Health Insurance Program (CHIP). On the website, you can search by location, dental specialty, language spoken and whether the dentist is accepting new patients.
- Adults: If you're over 21, your state's Medicaid website can help you figure out which dentists accept Medicaid and what kinds of dental care are covered in your state. If you are enrolled in a Medicaid managed care plan, you can log on to your insurance company's website to find available dentists.
- Seniors: If you have both Medicaid and a Medicare Advantage plan, you can find the list of dentists and covered services by logging into your Medicare Advantage plan account.
Be sure to check beforehand how much Medicaid pays for the care you need and how much you have to pay directly. Also check if Medicaid has a coverage limit in your state. If you need to, talk to your dental office about a payment plan or financing options.
Dental schools and clinics
Dental schools can also be good options for Medicaid patients. Many dental schools run clinics, which let the students get hands-on experience. Schools and their clinics can also be a good option for dental care without insurance.
Frequently asked questions
Does Medicaid cover dental care for adults?
Every state except Alabama offers some level of dental care for adults on Medicaid. However, the level of coverage changes depending on where you live. In some states, only emergency dental care is covered, while in others, more in-depth procedures like root canals or crowns are also covered.
Does Medicaid cover children's dental care?
Yes, state Medicaid programs are required to cover most dental services for people under the age of 21, as part of the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit.
Does Medicaid cover root canals?
Medicaid always covers root canals for children. For adults, Medicaid might cover root canals in some states. In states that offer extensive or comprehensive dental care for adults, root canals are likely to be a covered service. However, each state sets its own rules for dental coverage for adults. Check with your state's Medicaid office to be sure root canals are covered.
Sources
Info about state-specific Medicaid dental coverage for adults is from a 2022 survey by the National Academy for State Health Policy (NASHP) and a report by KFF. Other sources include the American Dental Association, Medicaid.gov, state Medicaid agencies and the U.S. Department of Health & Human Services (HHS).
About the Author

Senior Writer
Cate Deventer is a Senior Writer who specializes in health insurance, Medicare, auto and home insurance. She's been a licensed insurance agent since 2011.
She started her insurance career working as a customer service agent for State Farm. She later moved to an independent agency, where she worked with several insurance companies and hundreds of clients. She quoted policies, filed claims and answered insurance questions. In 2021, she pivoted her career and began writing about insurance for Bankrate. She moved to ValuePenguin in 2023 and began writing about health insurance and Medicare.
Cate has a passion for helping readers choose insurance to fit their needs. She enjoys knowing that her research and knowledge help people choose insurance products that make a positive difference in their lives.
How insurance helped Cate
Cate used her health insurance knowledge to navigate a surgery in 2023. Understanding how her policy worked let her focus on recovery instead of worrying about bills.
Expertise
- Health insurance
- Medicare & Medicaid
- Auto insurance
- Home insurance
- Life insurance
Credentials
- Licensed Life, Accident & Health Insurance Agent
- Licensed Property & Casualty Insurance Agent
Referenced by
- CBS
- NBC
- Wall Street Journal
Education
- BA, Theatre, Purdue University
- BA, English, Indiana University
Editorial note: The content of this article is based on the author's opinions and recommendations alone. It has not been previewed, commissioned or otherwise endorsed by any of our network partners.
