Your Guide to Employee Health Care Benefits
If your business has over 50 employees, you have to offer your workers health insurance.
Find Cheap Health Insurance Quotes in Your Area
If your business has fewer than 50 employees, you have the option to offer your employees health care benefits.
Employee health insurance costs an average of $746 per month to cover an individual. That's split between the business and the employee. Companies pay an average of $632 per month for employee coverage.
Do you have to offer your employees health insurance?
Legally, you have to offer your staff group health insurance if you have more than 50 full-time employees.
- Full-time employees: 30 hours per week or more
- Part-time employees: Under 30 hours per week
Depending on the number of part-time workers you have, they may count as full-time workers. That's because the government adds together the total number of hours worked by your part-time employees and divides that figure by 120 to get what's called a "full-time equivalent employee."
That means two employees who each work 15 hours per week would count as one full-time employee. The government adds your "full-time equivalent employees" to the number of your full-time workers when determining if you meet the 50-employee threshold.
You also need to make sure you offer coverage to at least 95% of your full-time employees and their dependents.
Do small businesses need to offer employee health insurance?
If you have fewer than 50 employees, you don't have to offer health insurance benefits. But there are some advantages that can make it a good idea.
A strong benefits package can help you get and keep employees. Plus, you can usually deduct your health insurance costs on your business's taxes. Companies with fewer than 25 employees can also get discounted rates through tax credits.
How does health insurance for employees work?
Health insurance for employees works as a single plan that covers most or all of the people in your business.
Health insurance for employees is also called group health insurance.
Companies typically pay for insurance benefits monthly. Employees pay for their portion of the cost directly through their paycheck. Costs depend on factors including where you are, how many employees you have, their ages and the tax benefits you get.
You can choose from several different types of insurance plans. The four most common types of plans are:
- Preferred Provider Organization (PPO): PPOs are the most flexible health insurance plan, but they're also the most expensive. You can see a specialist without a referral from your primary care doctor. You can also visit doctors who aren't in your network with a PPO, but you'll have to pay more to do so.
- Health Maintenance Organization (HMO): HMOs usually cost less than PPOs, but you can only see doctors in your network, and you'll need a referral before going to a specialist.
- Exclusive Provider Organization (EPO): EPO plans let you go to specialists without a referral, but coverage is limited to doctors in your network.
- Point of Service (POS): POS plans require referrals for certain services, but a POS still pays for some out-of-network doctors.
Each plan has a monthly cost, a deductible that the employee has to meet before the plan's full benefits start and a copay or coinsurance that the employee pays when they go to the doctor.
Watch out for very cheap group insurance plans. These plans may come with drawbacks, such as poor customer service, a small network of doctors or a history of denying claims at a higher than average rate.
How much does employee health insurance cost?
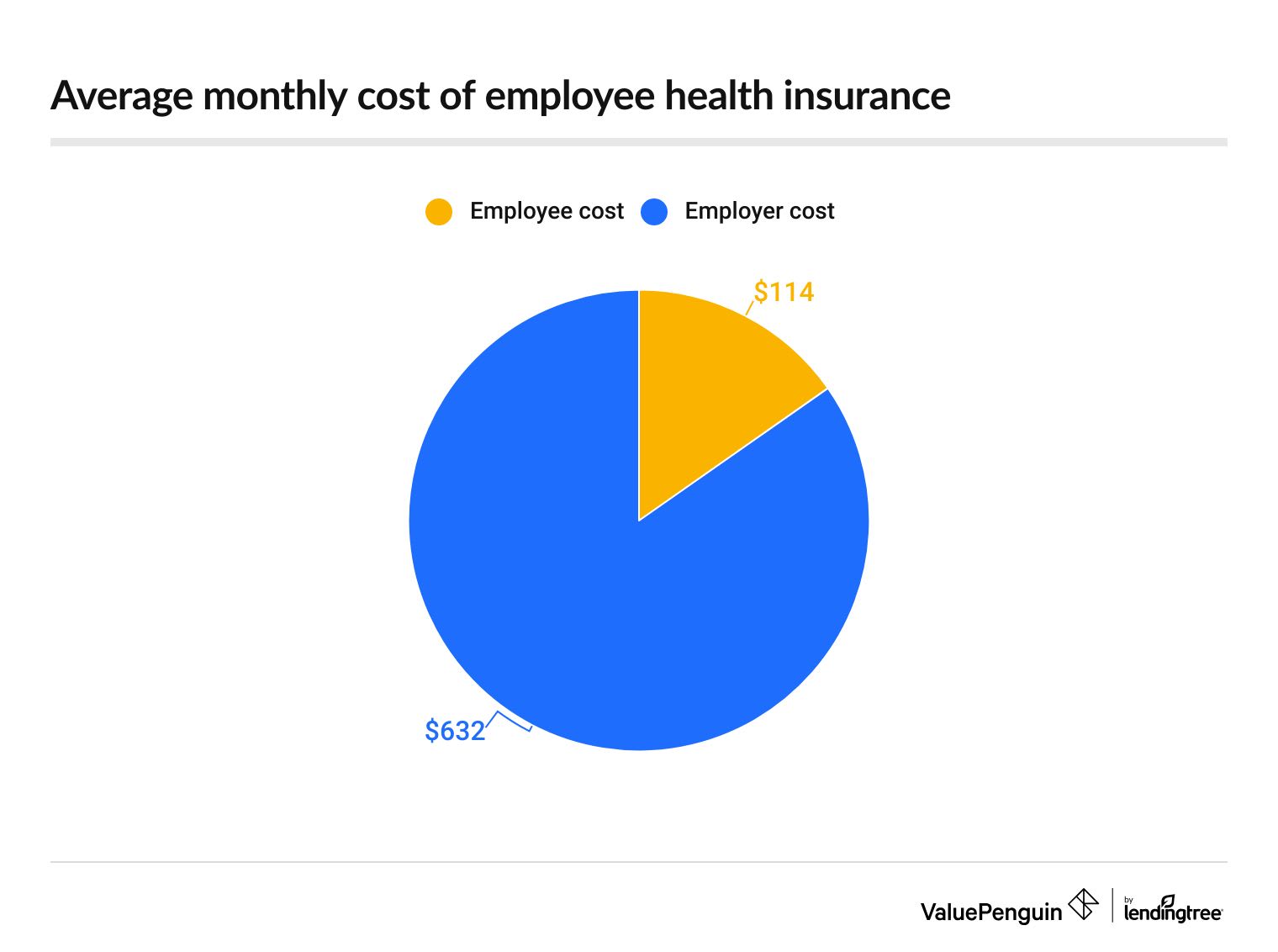
The cost of health insurance for an employee averages $746 per month for a single person.
That's typically split with the employee paying 16%, or $114 per month, and the employer paying the other $632 per month.
Find Cheap Health Insurance Quotes in Your Area
Employer coverage for families can be expensive. Even though workers with families pay a larger portion of the cost for their coverage than single employees, a company's portion of the monthly cost averages $1,606 per family.
Monthly cost of workplace health insurance
Individuals
Families
Employer cost | Worker cost | Total | |
|---|---|---|---|
| Average | $632 | $114 | $746 |
| HMO | $624 | $105 | $729 |
| PPO | $657 | $125 | $782 |
Employers contribute different amounts for the cost of employee health insurance. The level of benefits differs by employer, too
If you have more than 50 full-time employees, the lowest coverage level you can offer your employees is a Bronze health plan. This plan tier has the cheapest monthly costs, but your workers will pay more when they go to the doctor.
Tax benefits of offering employee health insurance
You can deduct what you pay for your employees’ health insurance on your business's taxes.
This lowers the amount you pay for federal and state taxes.
Plus, you may be eligible for the Small Business Health Care Tax Credit, which can lower your health insurance costs by up to half.
Small Business Health Care Tax Credit eligibility rules
- Have 25 or fewer full-time employees.
- The average employee salary is $62,000 or less.
- The business covers at least 50% of your employees' monthly costs
- All full-time employees are offered health care through SHOP.
Any tax credits you qualify for directly reduce the amount of taxes you need to pay. So if you owe $10,000 in taxes and get a $1,000 tax credit, then you're responsible for paying only $9,000 in taxes. Use HealthCare.gov's Small Business Health Care Tax Credit Estimator to see how much you could save.
Ways to save on employee health insurance
Paying for group insurance can be hard. But there are a few ways you can reduce those costs.
- Share costs with employees: Most employers share plan costs with employees. You can save by requiring your employees to pay a higher share of the plan's monthly costs or by choosing a plan tier that offers less coverage.
- Create your own health insurance group: If your employees are healthy and rarely get injured, you may want to consider a self-insurance plan. Instead of using a health insurance company, you set aside money each month for your employees’ health care. This means the risk of paying high health care costs falls on you as the employer. This may save money in the short-term, but one expensive health care bill can use up the entire budget. Companies typically work with an insurance agent to set this up and partner with a health insurance company to run the plan.
Where to find health insurance plans
To start, it's a good idea to find out what benefits your employees are looking for. For example, if a high percentage of your employees want strong dental benefits, you'll want a plan that includes this benefit. It's also helpful to know whether your employees value getting the lowest rate or if they'd prefer to pay more for better coverage.
Find Cheap Health Insurance Quotes in Your Area
1. Small Business Health Options Program (SHOP)
SHOP is a government-run health insurance marketplace for small-business owners. Each state has its own SHOP marketplace, but they're all similar. In order to use the marketplace, you need to meet the following requirements:
- Have one to 50 employees.
- Offer health care benefits to all employees who work at least 30 hours a week.
- Enroll 70% of the employees to whom you offer insurance.
- Have an office or employee in the state whose SHOP you'd like to use.
You can choose from four tiers of health insurance based on price and coverage. These include:
- Bronze plans have the cheapest monthly rates, but your employees will pay more when they go to the doctor.
- Silver plans offer a good mix between affordable rates and middle-of-the-road costs when your workers go to the hospital.
- Gold plans have high rates, but they'll pay for a large portion of your employees' medical bills.
- Platinum plans have the most expensive monthly rates and the best coverage of any plan tier.
The right plan for your employees will depend on their overall health and how much you want to spend. Bronze plans are usually a good choice if you have a young and healthy workforce. Silver plans make sense for most people, and you might consider a Gold or Platinum plan if many of your employees are older or dealing with health problems.
A higher plan tier can also help make your benefits package more attractive to new hires.
After picking a tier, your employees can visit the SHOP website and get their own plan.
2. Private health insurance marketplace
You can also find health insurance through private health insurance marketplaces. The quality and availability of plans depend on where you live, so it's a good idea to thoroughly research cost, coverage and customer service reputation before you choose a plan.
As with SHOP, companies can choose the plans that are available to employees and how much the employee will pay for the plan. Employees then choose the plan they want, and the employer gets a single bill for every employee. The marketplace typically offers services that help you understand and run the plan. For example, you can get support over the phone or by using HealthCare.gov to find a local agent, broker or assister.
3. Use a health insurance broker or agent
If you want help finding the best plan for your employees, consider hiring a health insurance broker. You can find a trusted broker through colleagues or SHOP. A good broker can help you navigate through the hard parts of picking a health insurance plan.
4. Professional employer organization (PEO)
With a PEO, you can let another company handle the administrative work related to getting and running a group health plan. PEOs are especially helpful for small businesses and startups because they handle insurance enrollment and claims paperwork. Plus, professional employer organizations can often save you money over what traditional health insurance companies charge.
5. HealthCare.gov marketplace if you're self-employed
If you're self-employed, consider the Affordable Care Act (ACA) Health Insurance Marketplace, also called Obamacare.
With ACA plans, you can see which tax credits, plans and discounts you can get.
Frequently asked questions
How does employer health insurance work?
Employer health insurance works by giving employees access to affordable coverage through a group health plan. The business is responsible for picking the group plan, and employees can choose to enroll.
Costs are typically split between the employer and the employee.
What are the rules for offering health insurance to employees?
You need to offer health insurance to your employees if you have 50 or more full-time workers. Keep in mind that part-time workers can be included in this number. For example, two employees who each work 15 hours per week count as one full-time employee.
How much does employee health insurance cost?
Employee health insurance costs an average of $746 per month for an individual. This cost is split between the employee and the company, with businesses typically paying $632 per month and workers paying $114 per month, on average.
Sources
Employee health insurance cost data came from Kaiser Family Foundation (KFF). Other sources include the IRS, the Bureau of Labor Statistics (BLS) and HealthCare.gov.
About the Author

Former Senior Writer
Talon Abernathy is a former ValuePenguin Senior Writer who specialized in health insurance, Medicare and Medicaid. He also contributed to other insurance verticals including home, renters, auto, motorcycle and flood insurance.
Talon came to ValuePenguin in 2023. Since his arrival, he's helped to expand the site's health insurance-related content offerings. He enjoys helping readers understand the ins and outs of America's all too complicated health insurance landscape.
Before coming to ValuePenguin, Talon worked as a freelance writer. His prior work has touched on a broad range of personal finance-related topics including credit-building strategies, small business incorporation tactics and creative ways to save for retirement.
Insurance tip
In many parts of the country, you can qualify for a free Silver health insurance plan if you meet certain income requirements. Government subsidies in the form of premium tax credits and cost-sharing reductions may mean you'll pay nothing for coverage.
Expertise
- Health insurance
- Medicare and Medicaid
- Flood insurance
- Homeowners insurance
- Renters insurance
- Auto and motorcycle insurance
Referenced by
- The Miami Herald
- Money.com
- MSN
- Nasdaq
- The Sacramento Bee
- Yahoo! Finance
Education
- BA, University of Washington
- Certificate in Copyediting, UC San Diego
Credentials
- Licensed Life & Disability Insurance Agent
- Licensed Property & Casualty Insurance Agent
Editorial note: The content of this article is based on the author's opinions and recommendations alone. It has not been previewed, commissioned or otherwise endorsed by any of our network partners.
