Cost of Medicare Part D in 2026 and How It Works
Medicare Part D, or Medicare drug coverage, is a part of Medicare that can help you pay for a variety of medications.
Compare Medicare Plans in Your Area
A Part D plan costs $62 per month, on average. You can buy a stand-alone Part D policy if you have Original Medicare (Part A and Part B), but not if you have Medicare Advantage (Part C).
How much does Medicare Part D cost for 2026?
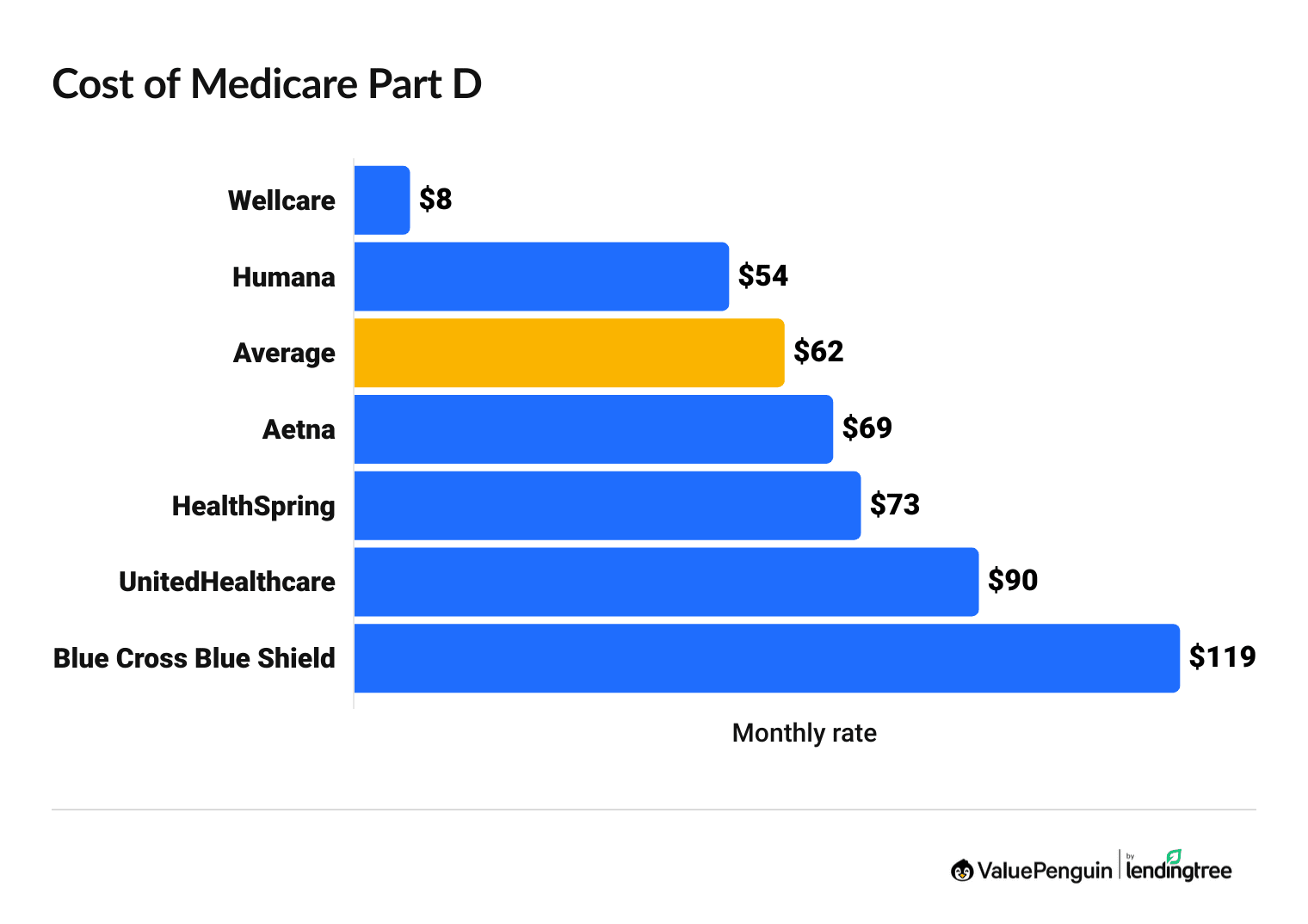
Medicare Part D costs $62 per month, on average, in 2026.
Rates vary depending on the company you choose. Wellcare has very cheap rates, while UnitedHealthcare and Blue Cross Blue Shield tend to be expensive.
Compare Medicare Plans in Your Area
These six companies are the only companies that sell stand-alone Part D plans, which means it's fairly easy to compare all your options when you're shopping.
Rates depend on where you live. For example, Blue Cross Blue Shield is generally expensive, but it is a cheaper-than-average option in Kansas.
Medicare Part D rates by company
Other Part D fees
Some customers also pay one or two extra fees on top of the cost for the Part D plan.
You might pay more if you sign up for Part D after you're first eligible. You might also pay a higher rate if you have a high income.
Medicare Part D late enrollment fee
If you decide to wait and join a Part D plan after your initial enrollment period ends, which is usually about three months after you turn 65, you'll pay an extra fee.
You'll be charged an extra 1% of the Part D base rate for every month that you delayed getting a Part D plan. The base rate changes from year to year, so your fee will also change. The late enrollment fee stays attached to your monthly rate for as long as you have a Part D plan.
For example, if you enroll in Part D 12 months after your initial enrollment period, your fee will be:
12% x $38.99, or $4.68
This means you will pay $4.68 extra every month. You'll pay this late enrollment fee for as long as you have Part D coverage, and it will change every year as the base rate changes. The fee is part of your monthly rate, and you pay it directly to your insurance company.
How to avoid the Medicare Part D late enrollment fee
You won't have to pay the late fee if you have prescription drug coverage from another plan, like a group health plan, private health insurance or a Medicare Advantage plan.
You can also avoid it in a few other ways:
- Enroll in Part D or a Medicare Advantage plan with drug benefits as soon as you become eligible.
- If you've lost your prescription plan due to a life-changing event such as an employment change, enroll in Medicare drug coverage within two months of losing coverage.
- If you think there's been a mistake, ask Medicare to reconsider within 60 days of learning about the fee. You can typically expect a reply within 90 days.
Compare Medicare Plans in Your Area
Part D rates for people with high incomes
You'll pay more for Part D if you make more than $109,000 per year as an individual or $218,000 if you file your taxes jointly.
This extra fee is called the income-related monthly adjustment amount (IRMAA). Your Part D rates for 2026 are based on the income you reported on your 2024 tax return.
Medicare Part D fees by income for 2026
How to calculate 2026 Part D extra costs
Let's say you are enrolled in a Part D plan for $60 per month for 2026, and you reported $110,000 of income in 2024. Based on your income, you would pay the cost of your plan ($60) plus an extra fee of $14.50, for a total Part D rate of $74.50.
You pay the $60 to your insurance company, while the $14.50 income adjustment fee goes directly to Medicare. The government typically takes this extra fee directly from your monthly Social Security payment. If you don't get Social Security or railroad retiree benefits, Medicare will send you a bill for the IRMAA fee.
Part D Extra Help
If you have a low income, you might be able to lower your monthly rate and how much you pay for prescriptions through the Extra Help program.
If you qualify for full Extra Help benefits, you won't have to pay a Part D monthly rate or a deductible. And if you get your medications at certain pharmacies, you'll only pay up to $5.10 for generic medications and up to $12.65 for name-brand medications.
Part D Extra Help eligibility
You can apply for Extra Help online through the Social Security Administration website.
How does Medicare Part D work?
Medicare Part D helps you pay for prescription medications.
Part D is sold by private insurance companies, unlike Parts A and B, which come from the federal government. All policies have to offer a standard level of coverage. That means every plan will pay for at least two different drugs for each drug category.
If you need coverage for a specific medication, it is important to look at the list of prescription drugs, also called a drug formulary, that a Part D plan covers. You can find coverage information in the insurance company's plan documents or by visiting the Medicare Part D plan finder tool.
Medicare Part D groups drugs together with similar out-of-pocket costs. Inside these groups, name-brand drugs are either labeled "preferred" or "nonpreferred." Nonpreferred drugs typically have the highest copays. Generics usually have the lowest copays.
If a drug falls into the nonpreferred category, it's because the insurance company found a lower-cost version that serves the same purpose.
What you'll pay for prescriptions with Medicare Part D
Along with the monthly rate of your Part D plan, you'll pay part of the cost of the drugs you buy.
You're usually responsible for the full cost of your medications until you meet your annual deductible.
Then you either pay a certain dollar amount each time you pick up a prescription, also called a copay, or a percentage of your total bill, also called coinsurance. For example, you might pay $10 each time you get a prescription drug or you might be responsible for 20% of the drug's cost.
Your out-of-pocket costs change depending on how much you've already paid. There are three stages to this process.
Deductible stage: During this time, you pay the full price for prescriptions until your costs reach a certain amount set out in your plan. The maximum deductible for 2026 is $615, but your plan may charge less.
Initial coverage stage: After you meet your deductible, you enter the initial stage. While in this stage, you pay 25% of the cost for prescriptions until you've paid $2,100 in total. Your plan pays the other 75% of the cost for your medications.
Catastrophic coverage stage: The catastrophic benefit period kicks in after you've paid $2,100 in a single calendar year. In this phase, you don't pay anything when you go to the pharmacy for the rest of the calendar year.
You may have heard about the Part D "donut hole" or "coverage gap." This used to be a phase of coverage between the initial and catastrophic phases where you had to pay the full cost of your medications.
The donut hole was closed completely in 2025. Now, Part D coverage phases move straight from the initial phase into the catastrophic phase once you've hit $2,100 in medication costs.
Example
Deductible stage
| Who pays | You |
| What you pay | Up to $615 |
| What the plan pays | $0 |
Initial coverage stage
| Who pays | You and your plan |
| What you pay | 25% of the cost of your medications until your total spending reaches $2,100 |
| What the plan pays | 75% of the cost for your medications |
Catastrophic coverage stage
| Who pays | Your plan |
| What you pay | $0 |
| What the plan pays | 100% of the cost of your covered medications |
Medicare Part D eligibility and enrollment
To get Part D, you first have to sign up for Medicare Parts A and B.
To do this, you have to meet one of the following requirements:
- Be over the age of 65
- Have a disability if you are under the age of 65
- Have end-stage renal disease (kidney failure)
- Have Lou Gehrig's disease (ALS)
You have seven months to sign up for Part D when you're first eligible, so you avoid any late fees. You can sign up for Part D starting three months before your 65th birthday, in your birth month and for three months after. If your birthday falls on the 1st of the month, your enrollment period starts four months before your birth month and ends two months after.
Do I need Medicare Part D?
You probably need a Part D plan if you have Original Medicare.
That's because Original Medicare (Parts A and B) doesn't usually give you coverage for medications unless you're in the hospital or a doctor's office. Even if you don't take any prescriptions now, there's a good chance that you will at some point in your life. Some medications can be incredibly expensive, which makes a Part D plan a smart choice.
Because Medicare Part D has a late enrollment fee that lasts for as long as you have Medicare coverage, it's a good idea to enroll in a Part D plan when you turn 65.
Choosing your Medicare Part D plan
Use your prescription drug needs to guide your Part D plan choice. For example, if you mostly use generic drugs, then review the drug lists for each plan, and pick a policy with small copayments for generic, lower-tier drugs.
If you need coverage for a very specific drug, then you should carefully review the drug list, called a formulary, to make sure the drug you need will be covered.
Medicare Advantage: An alternative to Medicare Part D
Medicare Advantage, also called Medicare Part C, lets you bundle Parts A, B and usually D coverage in a single plan.
However, not all Medicare Advantage plans have drug coverage. Before you buy a plan, make sure you're looking at plans that have prescription drug coverage included. Check your Part C plan's list of covered drugs for any medications you're currently taking before you sign up.
And if you don't like your Medicare Advantage plan, you won't have to pay a late enrollment fee if you switch back to Original Medicare as long as you buy a Part D policy within 63 days.
Medicare Advantage (Part C) plans are run by private insurance companies like UnitedHealthcare and Humana. You can save money on your Medicare costs by picking a Medicare Advantage plan with no monthly rate.
Keep in mind that Medicare Advantage plans often limit you to a network of doctors. By contrast, Original Medicare lets you see any doctor who accepts Medicare nationwide.
Frequently asked questions
What is the average monthly cost of Medicare Part D?
For 2026, the cost of Medicare Part D is $62 per month, on average. These Medicare drug plans pay for your medications if you have Original Medicare (Parts A and B).
Is Medicare Part D deducted from your Social Security?
You can have your Part D rates deducted from your Social Security benefits, but you have to arrange that with the company you buy a plan from. You can also pay the insurance company directly from your Part D plan. If you have a high income and pay an IRMAA fee, the fee will be taken directly out of your Social Security benefits.
Is there a fee for Part D Medicare?
Yes, there are fees associated with Part D. The first is the monthly rate for the plan you pick. Like other insurance plans, Part D plans also have deductibles, copays and coinsurance that you pay, as well, when you pick up prescriptions. If you make more than $109,000 per year, you'll pay an extra fee for Part D. And if you sign up late, you'll pay an extra fee, as well.
Is it worth getting Medicare Part D?
Yes, you should get prescription drug coverage through Medicare Part D if you're enrolled in Original Medicare. Even if you don't need prescription drug coverage now, you should sign up within three months of your 65th birthday to avoid paying a late penalty fee.
What can I do to avoid Part D late enrollment fees?
To avoid late enrollment fees, join a Part D plan (or a Medicare Advantage plan with drug coverage) when you first become eligible for Medicare. Even if you don't take prescriptions now, you'll have coverage when you need it without paying a fee.
Similarly, enroll in Part D or Medicare Advantage as soon as you lose other health insurance with drug coverage.
Methodology
Cost, eligibility and enrollment information for Medicare Part D came from Medicare's website, Medicare.gov, as well as from the Centers for Medicare & Medicaid Services (CMS). Company rates are grouped by consumer brand and include subsidiaries. Averages are based on plans in all 50 states and Washington, D.C.
About the Author

Senior Writer
Cate Deventer is a Senior Writer who specializes in health insurance, Medicare, auto and home insurance. She's been a licensed insurance agent since 2011.
She started her insurance career working as a customer service agent for State Farm. She later moved to an independent agency, where she worked with several insurance companies and hundreds of clients. She quoted policies, filed claims and answered insurance questions. In 2021, she pivoted her career and began writing about insurance for Bankrate. She moved to ValuePenguin in 2023 and began writing about health insurance and Medicare.
Cate has a passion for helping readers choose insurance to fit their needs. She enjoys knowing that her research and knowledge help people choose insurance products that make a positive difference in their lives.
How insurance helped Cate
Cate used her health insurance knowledge to navigate a surgery in 2023. Understanding how her policy worked let her focus on recovery instead of worrying about bills.
Expertise
- Health insurance
- Medicare & Medicaid
- Auto insurance
- Home insurance
- Life insurance
Credentials
- Licensed Life, Accident & Health Insurance Agent
- Licensed Property & Casualty Insurance Agent
Referenced by
- CBS
- NBC
- Wall Street Journal
Education
- BA, Theatre, Purdue University
- BA, English, Indiana University
Editorial Note: We are committed to providing accurate content that helps you make informed financial decisions. Our partners have not endorsed or commissioned this content.
